Let's be real, ticks are a pain. A tiny, eight-legged pain that can turn a perfect hike, camping trip, or even an afternoon in your own backyard into a source of anxiety. You've probably heard the scary stories about Lyme disease. Maybe you've found one on your dog or felt that dreaded itch on your scalp after being outdoors. I get it. I've spent countless hours in tick-heavy areas, and the paranoia is real. But here's the thing: fear comes from the unknown. Once you understand ticks—how they operate, how to spot them, and exactly what to do if you find one—that anxiety transforms into simple, actionable preparedness. This guide is about making that shift.
What You'll Find in This Guide
Know Your Enemy: The Most Common Ticks
Not all ticks are the same. Different species carry different diseases and are active at different times. Misidentifying a tick can lead to unnecessary worry or, worse, misplaced complacency. Here are the two you're most likely to encounter in many regions, especially in North America and Europe.
The Black-Legged Tick (Deer Tick)
This is the one that gets all the headlines. It's the primary vector for Lyme disease, but also anaplasmosis and babesiosis. Adults are reddish-brown with dark black legs. The nymphs, which are most active in spring and summer and are about the size of a poppy seed, are responsible for the majority of Lyme disease cases. People often miss them.
The American Dog Tick
Larger and more common in open fields and along trails. Males have a mottled gray pattern, while females have a distinct off-white scutum (shield) on their backs. These ticks rarely transmit Lyme but are the main vector for Rocky Mountain Spotted Fever and tularemia. Their larger size makes them easier to spot, which is a small mercy.
Pro Tip: The "Lone Star Tick," identifiable by a single white dot on the female's back, is expanding its range. It's notorious for causing an allergy to red meat (alpha-gal syndrome). If you develop hives or stomach issues hours after eating beef or pork and have been in tick country, mention this to your doctor.
| Tick Species | Key Identifying Feature | Primary Diseases | Active Season |
|---|---|---|---|
| Black-Legged (Deer) Tick | Dark black legs, reddish-brown body | Lyme disease, Anaplasmosis, Babesiosis | Nymphs: Spring/Summer; Adults: Fall/Spring |
| American Dog Tick | Mottled gray (male), white scutum (female) | Rocky Mountain Spotted Fever, Tularemia | Spring, Summer |
| Lone Star Tick | Single white dot on female's back | Alpha-gal syndrome (red meat allergy), STARI | Spring through Fall |
Your Tick Prevention Strategy (It's More Than Spray)
Prevention is a layered defense, not a single product. Relying solely on bug spray is like locking only your front door. Here's the system I use and recommend.
Personal Protection: Use an EPA-registered repellent containing DEET (20-30%), picaridin, or IR3535. For clothing and gear, treat them with a product containing permethrin. This is a game-changer. Permethrin bonds to fabric fibers and kills ticks on contact. You can buy pre-treated clothing or treat your own (follow label instructions carefully—it's for fabric, not skin). Tuck your pants into your socks. It looks dorky, but it creates a physical barrier.
Environmental Management: Keep your yard trimmed. Clear leaf litter and tall grasses, especially around play areas and patios. The Centers for Disease Control and Prevention (CDC) notes that creating a 3-foot wide barrier of wood chips or gravel between lawns and wooded areas can help. Consider managing deer populations, as they are key hosts for ticks like the black-legged tick.
The Critical Routine: The Post-Adventure Check. This is non-negotiable. As soon as you come inside, throw all your clothes into a dryer on high heat for 10 minutes. The dry heat kills ticks that washing alone might not. Then, do a full-body tick check. Use a mirror or partner up. Key spots ticks love: behind the knees, in the groin, under the arms, in and around the ears, belly button, and scalp. Do this check again the next morning. Nymphs are so small they can feel like a speck of dirt.
How to Safely Remove a Tick: The Right Way
You found one. It's attached. Don't panic, and for heaven's sake, ignore the old wives' tales. No matches, no nail polish, no petroleum jelly. Those methods can cause the tick to regurgitate pathogens into you.
The Tool: Fine-tipped tweezers. Not household tweezers with slanted ends. The fine tips allow you to grasp the tick as close to the skin's surface as possible. You can buy dedicated tick removal tools, but good tweezers work perfectly.
The Steps:
- Grasp the tick with the tweezers, getting as close to your skin as you can. Get a firm grip on its head/mouthparts.

- Pull upward with steady, even pressure. Don't twist or jerk. You want to pull the tick out cleanly, like lifting a splinter.
- Clean the bite area and your hands thoroughly with rubbing alcohol or soap and water.
- Dispose of the tick. Don't crush it with your fingers. Flush it down the toilet, or place it in a sealed bag/container with alcohol. I recommend saving it in a bag labeled with the date—it can be tested if you get sick.
What if the head breaks off and stays in your skin? Try to remove it with the tweezers. If you can't, leave it alone and let the skin heal. Your body will expel it like a small splinter. Just keep the area clean.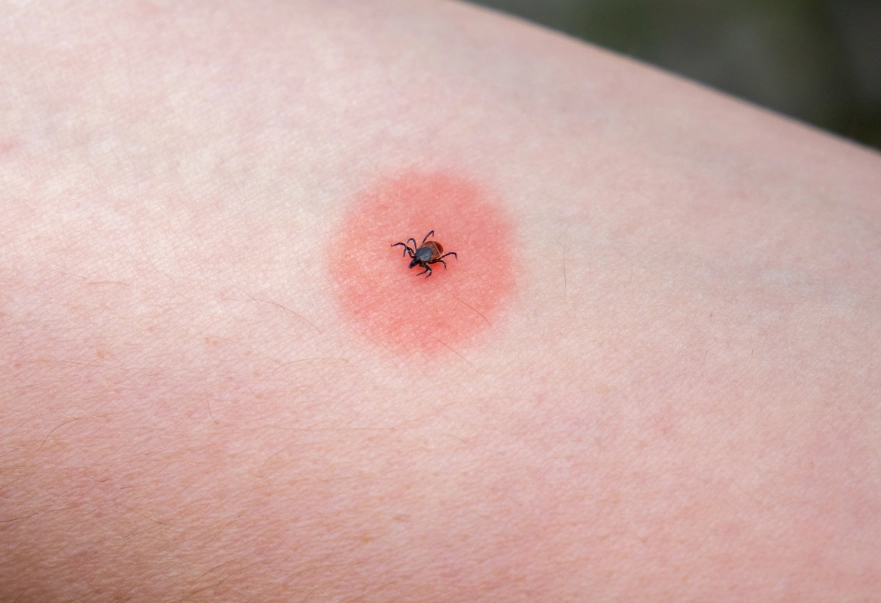
After the Bite: Symptoms and Monitoring
Removal is step one. Step two is vigilant observation for the next 30 days. Document the bite. Take a photo of the spot and note the date.
The Lyme Disease Rash (Erythema Migrans): Not everyone gets the classic "bull's-eye" rash. It can be a solid red expanding rash, often at the bite site. It usually appears 3-30 days after the bite and can expand to several inches wide. It's typically not itchy or painful. If you see any expanding rash, see a doctor immediately. According to the World Health Organization (WHO), early diagnosis of Lyme is crucial for effective treatment.
Flu-Like Symptoms: Fever, chills, headache, fatigue, muscle and joint aches can be early signs of several tick-borne illnesses, not just Lyme.
My rule of thumb: If you develop an unexplained fever or flu-like illness within a month of a known tick bite or being in a tick area, tell your doctor about the possible tick exposure. It changes the diagnostic picture completely.
Your Tick Questions, Answered
What's the single biggest mistake people make when removing a tick?
Using heat, petroleum jelly, or nail polish to try and "suffocate" the tick. This method stresses the tick, dramatically increasing the chance it will regurgitate its gut contents (and any pathogens) directly into your bloodstream. The only correct tool is a pair of fine-tipped tweezers, grasping as close to the skin as possible and pulling straight up with steady pressure.
How long does a tick need to be attached to transmit Lyme disease?
The transmission risk for Lyme disease bacteria (Borrelia burgdorferi) is very low if the tick is attached for less than 24 hours. Risk increases significantly after 36-48 hours of attachment. This is why performing a daily, thorough tick check is your most powerful defense—it gives you a window to find and remove them before they become a serious health threat.
I found a tick crawling on my clothes but not attached. Am I still at risk?
The immediate risk of disease transmission is zero if the tick did not bite. However, its presence is a major red flag. It means you were in a tick habitat, and others could be on you, your gear, or pets. Immediately treat your clothing with high heat (tumble dry for 10 minutes on high) and conduct a full-body check on yourself and anyone with you. Consider the encounter a successful early warning.
What should I do with the tick after I remove it?
Don't just flush it. Place it in a sealed plastic bag or small container with a bit of rubbing alcohol. Note the date and location on the bag. If you develop any unusual symptoms like a rash or fever in the next 30 days, this preserved tick can be sent for testing (through some state health departments or private labs), which can help your doctor make a faster, more accurate diagnosis.